(ITUNES OR LISTEN HERE)
The Society of Critical Care Medicine (SCCM) and the European Society of Intensive Care Medicine (ESICM) redefined sepsis with the Third International Consensus Definitions for Sepsis and Septic Shock (Sepsis-3). Sepsis is life-threatening organ dysfunction due to dysregulated host responses to infection. Septic shock is a subset of sepsis where underlying circulatory and cellular/metabolic abnormalities are profound enough to substantially increase mortality [2].
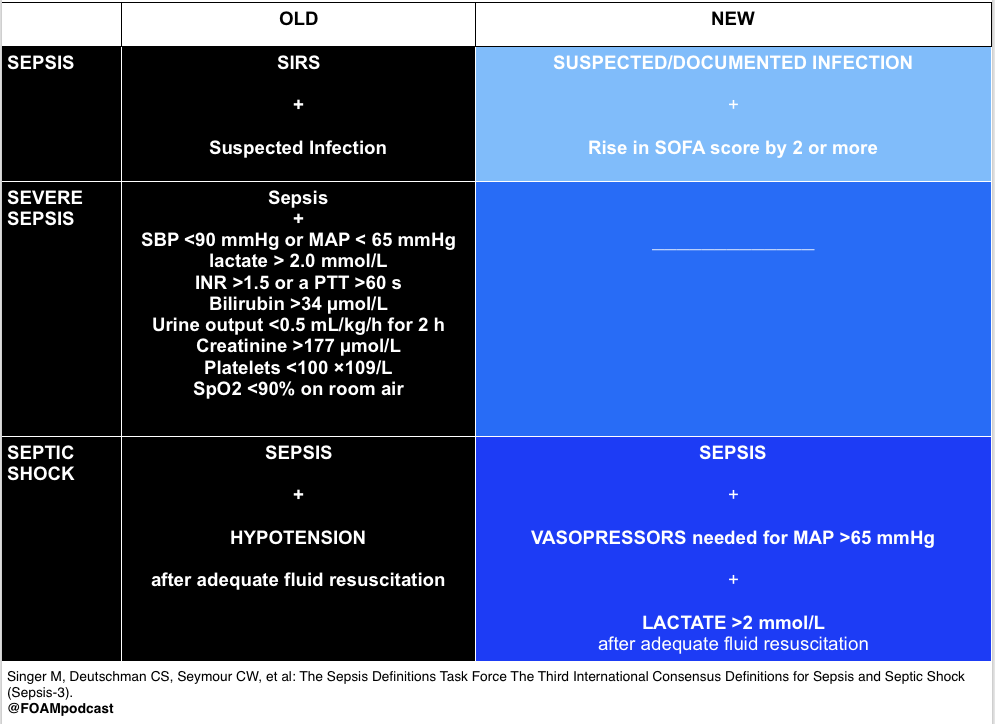
2003 vs 2016 Definitions of Sepsis [1-4]
Systemic Inflammatory Response Syndrome (SIRS) is out.
- Includes normal responses to infection (eg. fever and tachycardia is not dysregulated infection; it’s just infection)
- SIRS even MISSES up to ⅛ very septic ICU pts (NEJM 2015) [5].
qSOFA is in. a qSOFA score of 2 or 3 or a rise in the SOFA score of 2. The SOFA score requires a ton of lab values so the authors wanted something that could be assessed at triage, hence the quick SOFA score (qSOFA). The authors derived and retrospectively validated this score and compared it to SIRS in a cohort of 148,907 patients [3]

Issues:
- Unclear how to interpret studies (EGDT through ProCESS, PROMISE, ARISE) with new definitions.
- CMS is not going to adapt.
- Not endorsed by ACEP or SAEM as emergency providers were not included.
- qSOFA has not been prospectively validated. It’s unclear how it will perform in this fashion
Notes: Sepsis rates have increased over the past 10 years and it appears that mortality has decreased. However, less sick patients are included in this. It appears that the Sepsis 3 authors were hoping for a more specific definition.
References:
- Levy MM, Fink MP, Marshall JC. 2001 SCCM/ESICM/ACCP/ATS/SIS International Sepsis Definitions Conference. Critical care medicine. 31(4):1250-6. 2003.
- Singer M, Deutschman CS, Seymour CW, et al: The Sepsis Definitions Task Force The Third International Consensus Definitions for Sepsis and Septic Shock (Sepsis-3).
AMA. 2016;315(8):801-810. doi:10.1001/jama.2016.0287.
- Seymour CW, Liu V, Iwashyna TJ, et al. Assessment of clinical criteria for sepsis: For the Third International Consensus Definitions for Sepsis and Septic Shock (Sepsis-3).JAMA. 2016;315(8):762-774. doi:10.1001/jama.2016.0288.
- Shankar-Hari M, Phillips G, Levy ML, et al.Developing a New Definition and Assessing New Clinical Criteria for Septic Shock: For the Third International Consensus Definitions for Sepsis and Septic Shock (Sepsis-3). (JAMA, Feb 22, 2016).
- Kaukonen KM, Bailey M, Bellomo R. Systemic Inflammatory Response Syndrome Criteria for Severe Sepsis. The New England journal of medicine. 373(9):881. 2015.
Great post, guys! Thanks!
Minor detail: Url for 4th reference (Shankar-Hari et al) same as for 3rd. Should be http://jama.jamanetwork.com/article.aspx?articleid=2492876.
All the best. /Mads
This was a problem on the original JAMA site (only redirected to Seymour article). This is fixed. Our apologies for the delay, the post was written just prior to articles being released by JAMA (thus DOI etc was unavailable) and we were on clinical shift. Now fixed. Thanks!
Great post, guys! Thanks!
Minor detail: Url for 4th reference (Shankar-Hari et al) same as for 3rd. Should be http://jama.jamanetwork.com/article.aspx?articleid=2492876.
All the best. /Mads
This was a problem on the original JAMA site (only redirected to Seymour article). This is fixed. Our apologies for the delay, the post was written just prior to articles being released by JAMA (thus DOI etc was unavailable) and we were on clinical shift. Now fixed. Thanks!
I’m not really sure what the point of redefining sepsis is. I understand that under the current definition, SIRS + possible source of infection, that we treat almost every patient who comes into the hospital as septic or potentially septic. This has lead to aggressive and unnecessary treatment for patients who have a bad but not life threatening infection and for patients with no infection. I understand that it is time to start scaling back how aggressive we are to treat septic or possibly septic patients. What i dont understand is how simply redefining sepsis, when it is clearly the implementation of evidence based lacking guidelines that’s leading to aggressive treatment, will really change anything.
I’m not really sure what the point of redefining sepsis is. I understand that under the current definition, SIRS + possible source of infection, that we treat almost every patient who comes into the hospital as septic or potentially septic. This has lead to aggressive and unnecessary treatment for patients who have a bad but not life threatening infection and for patients with no infection. I understand that it is time to start scaling back how aggressive we are to treat septic or possibly septic patients. What i dont understand is how simply redefining sepsis, when it is clearly the implementation of evidence based lacking guidelines that’s leading to aggressive treatment, will really change anything.
This new definition of sepsis fails to take into account the role SIRS plays in clinical judgement in deciding whether patients have an infection or source of infection. Reading between the lines the new sepsis definition really is just SIRS + qsofa + altered mentation + hypotension + tacyhpnea. It really is just a different way of defining what was previously called severe sepsis. It calls for discarding SIRS without acknowledging the role SIR plays.
This new definition of sepsis fails to take into account the role SIRS plays in clinical judgement in deciding whether patients have an infection or source of infection. Reading between the lines the new sepsis definition really is just SIRS + qsofa + altered mentation + hypotension + tacyhpnea. It really is just a different way of defining what was previously called severe sepsis. It calls for discarding SIRS without acknowledging the role SIR plays.
One distinction made by the task force is that they recommended using GCS <15 rather than <=13, despite the qSOFA definition.