Episode 7 (iTunes or Listen Here)
The Free Open Access Medical Education (FOAM)
Impact apnea –people who sustain traumatic brain injury often have associated apnea. Support their airway because this could lead to arrest. Bystander support is crucial.
Right Ventricular Myocardial Infarction (RVMI)– Think about this in any inferior MI situation. Give fluids, these patients are preload dependent and need the cath lab.
Right Ventricular Heart Failure – OH CRAP.
- Optimize Oxygenation, Hemodynamics, Contractility, Rate/rhythm, Afterload, and Preload
- Give fluids, but not too much. Inotropes and vasopressors are often necessary. These guys like milrinone and epinephrine.
The Bread and Butter
We summarize some key topics from the following readings, Tintinalli (7e) Chapters 53, 57; Rosen’s (8e) Chapters 78, 81…but, the point isn’t to just take our word for it. Go enrich your fundamental understanding yourself!
RVMI – often associated with inferior MIs and can carry increased morbidity/mortality.
ECG pearls –
- look for ST elevation in lead III greater than lead II or lead V1 (especially with ST depression in V2.
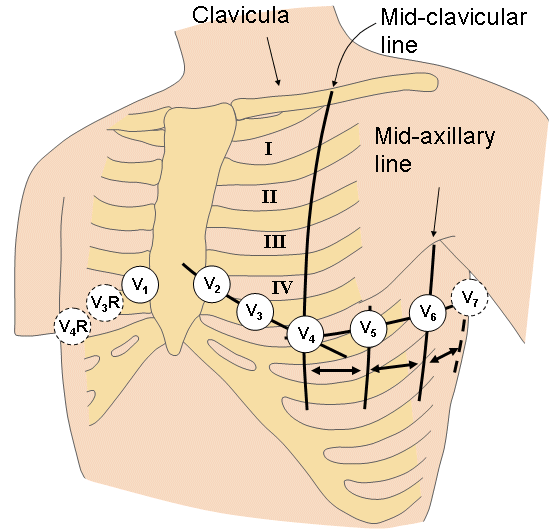
- Right sided leads – elevation in V4R most specific but elevation in V3R-6R are indicative of RVMI. Keep V1 and V2
Treatment – RVMI is preload dependent so they need fluid. Too much fluid may cause the RV to impinge on the LV.
Acute Heart Failure (WikEM)
- Give nitrates, which decrease preload, before diuretics. Diuretics are only indicated in volume overloaded patients, and many patient simply have fluid shifts and are overall euvolemic or have decreased plasma volume. Thus, in some patients, diuretics may be harmful.
- Use non-invasive ventilation
- BNP. The boards and ACEP recommend it but randomized clinical trials have not consistently demonstrated a benefit in the Emergency Department (Carpenter et al)
Right vs Left Sided Heart Failure – this distinction is someone artificial as chambers are interdependent in series.
- Left-sided failure – pulmonary symptoms (dyspnea and orthopnea)
- Right-sided failure have systemic venous congestion(pedal edema and hepatomegaly)
High Output Failure – conditions with excess cardiac output
- Causes – increased preload (excess mineralocorticoids, fluid/salt retention), decreased systemic vascular resistance (pregnancy, cirrhosis, severe anemia, beriberi, thyrotoxicosis, Paget’s disease, or vasodilator medications), or tachycardia and persistent beta-adrenergic stimulation.
- Treatment – correct underlying cause
Generously donated Rosh Review questions (scroll for answers)
Question 1. [polldaddy poll=8168396]
Question 2. A 73-year-old man presents to the ED with progressive shortness of breath for two days without chest pain. The patient has a history of hypertension controlled with hydrochlorothiazide, but has been noncompliant with his medications. In the ED, his vital signs are BP 186/102, HR 108, RR 34, and oxygen saturation 90% on room air. On exam, the patient has pulmonary crackles midway up both lung fields, jugular venous distension, and pitting edema of his lower extremities. A chest X-ray depicts increased interstitial markings and an enlarged cardiac silhouette. An ECG shows sinus tachycardia. [polldaddy poll=8168406]
Question 3. [polldaddy poll=8169897]
References:
O’Brien JF. Heart Failure. Rosen’s Emergency Medicine (8e). Chapter 81, 1075-1090.e7
Hollander JE, Diercks DB. Chapter 53: Acute Coronary Syndromes: Acute Myocardial Infarction and Unstable Angina.”Tintinalli’s Emergency Medicine: A Comprehensive Study Guide, 7e. New York, NY: McGraw-Hill; 2011. p 367-385
Peacock WF. Chapter 57: Congestive Heart Failure and Acute Pulmonary Edema. Failure. Tintinalli’s Emergency Medicine: A Comprehensive Study Guide, 7e. New York, NY: McGraw-Hill; 2011 p 404-414
Answers:
Question 1. D. This patient presents with symptoms of acute decompensated heart failure (ADHF) and should be started on nitroglycerin therapy immediately. Patients with ADHF present with shortness of breath, increased work of breathing, tachycardia, hypoxia, crackles on lung examination and jugular venous distension. These patients experience acute worsening of left ventricular function and output secondary to a number of mechanisms including increased systemic vascular resistance. Therapy focuses on reduction of preload to decrease the flow of blood into the lungs and afterload reduction to increased the effectiveness of the left ventricle. Both of these goals can be accomplished through the administration of nitroglycerin. At lower doses, nitroglycerin acts as a peripheral vasodilator and increases venous capacitance leading to decreased preload. At higher doses, nitroglycerin causes arterial vasodilation leading to decreased afterload. Because of its rapid onset of action, nitroglycerin is the first line medication in patients with ADHF. Furosemide (A) may be useful in patients with volume overload and ADHF but this represents less than half of patients with ADHF. Additionally, the effects are delayed. Heparin (B) can be given in cases of ischemia induced ADHF but will not yield any immediate benefits. Morphine (C) was historically used as a preload reducer but has been associated with increased morbidity in patients with ADHF and is no longer recommended.
Question 2. A . This patient is in acute heart failure with pulmonary edema. The clinical presentation of heart failure includes shortness of breath, jugular venous distension, crackles and rales, peripheral edema, S3 gallop, orthopnea, and paroxysmal nocturnal dyspnea. A chest X-ray may show an enlarged cardiac silhouette, Kerley B lines suggesting pulmonary edema, and pulmonary vessel cephalization. Labs may show an elevated plasma brain natiuretic peptide (BNP). Management of heart failure with acute pulmonary edema begins with addressing the ABCs.Noninvasive respiratory therapy, such as bilevel positive airways pressure (BiPAP) or continuous positive pressure airway (CPAP) is the most appropriate next step in management. Noninvasive positive pressure ventilation increases oxygenation, decreases the worth of breathing, and decreases preload and afterload. In addition to BiPAP, adjunctive medications include nitrates, diuretics, morphine sulfate, and position the patient sitting up. Nitrates act as venous and arterial vasodilators and help to reduce preload and afterload. Morphine sulfate is thought to decrease oxygen consumption by decreasing catecholamines, decrease preload from mild vasodilator effects and decreases pain and anxiety. However, there are some studies that link the use of morphine sulfate to an increased mortality. Furosemide can be used in patients with evidence of fluid retention (JVD, extremity edema). Pulmonary edema secondary to heart failure usually responds well to preload and afterload reduction with noninvasive ventilation and nitroglycerin. If the patent continues to deteriorate then intubation (C) may be necessary. A myocardial infarction is less likely given the lack of chest pain and ECG that does not reveal ST-segment elevations. Therefore, activation of the cath lab (B) is unnecessary. Hydrochlorothiazide (D) has no role in the acute management of pulmonary edema. Once stabilized, the patient can resume his daily medications.
Question 3. Correct Answer ( C ) Atrioventricular (AV) conduction blocks occur in 25%–30% of patients with acute myocardial infarction. A narrow complex third-degree AV block in the setting of an inferior wall MI is usually transient and resolves spontaneously. Other AV blocks associated with a favorable prognosis include first-degree heart block and second-degree Mobitz type I (Wenckebach). Patients with a new left bundle branch block (A) in the setting of an acute MI are more likely to develop CHF, AV block, and ventricular fibrillation and have an overall increased mortality. Left posterior hemiblock (B) is associated with a large infarct size, increased risk of cardiogenic shock, and increased mortality. A new right bundle branch (D)in the setting of an anterior wall MI is associated with an increased risk of developing complete AV block and cardiogenic shock.