We cover a talk from Bryan Hayes (@PharmERToxGuy) at the American College of Emergency Physicians #ACEP19 conference on medications we use in the ED that have….black box warnings
Deep dive on fluoroquinolones and aortic dissection/aneurysm
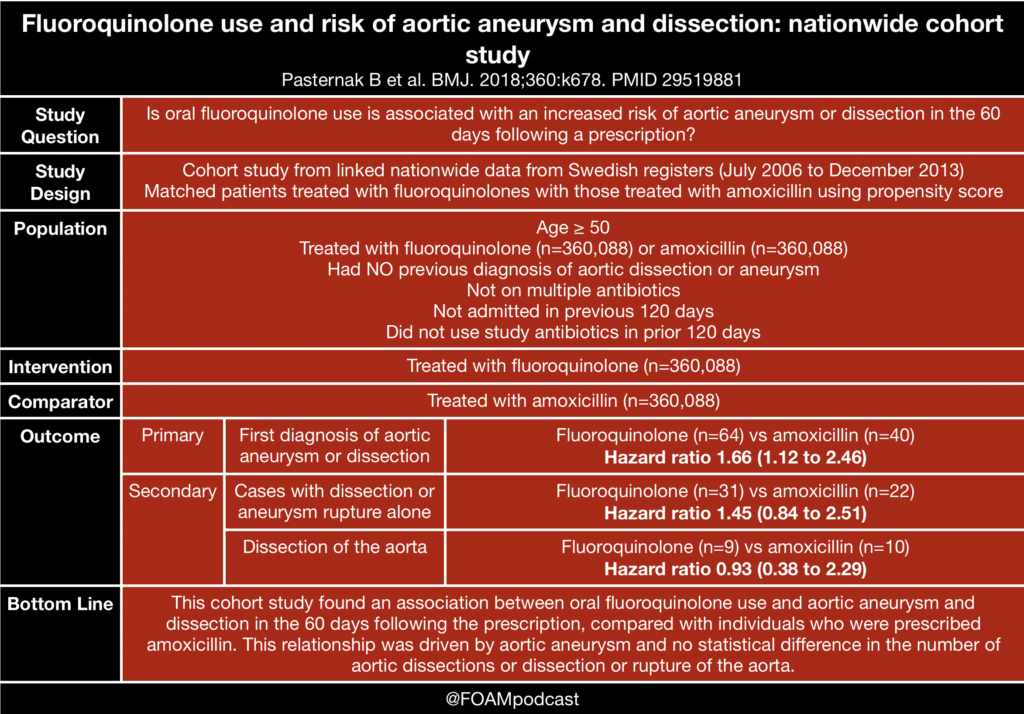


We cover a talk from Bryan Hayes (@PharmERToxGuy) at the American College of Emergency Physicians #ACEP19 conference on medications we use in the ED that have….black box warnings
Deep dive on fluoroquinolones and aortic dissection/aneurysm



Vaping associated lung injury (VALI) has become a frequent topic in the news in the United States (US). The Centers for Disease Control and Prevention (CDC) has released new guidance for clinicians that we review in this episode. We also discuss problems with widespread concern (potential over-screening and radiation exposure) as well as the available evidence on diagnosis and treatment of VALI.
References:
Insulin is a mainstay in the emergent treatment of hyperkalemia but comes at the cost of increased risk of hypoglycemia, which is quite common.
References:
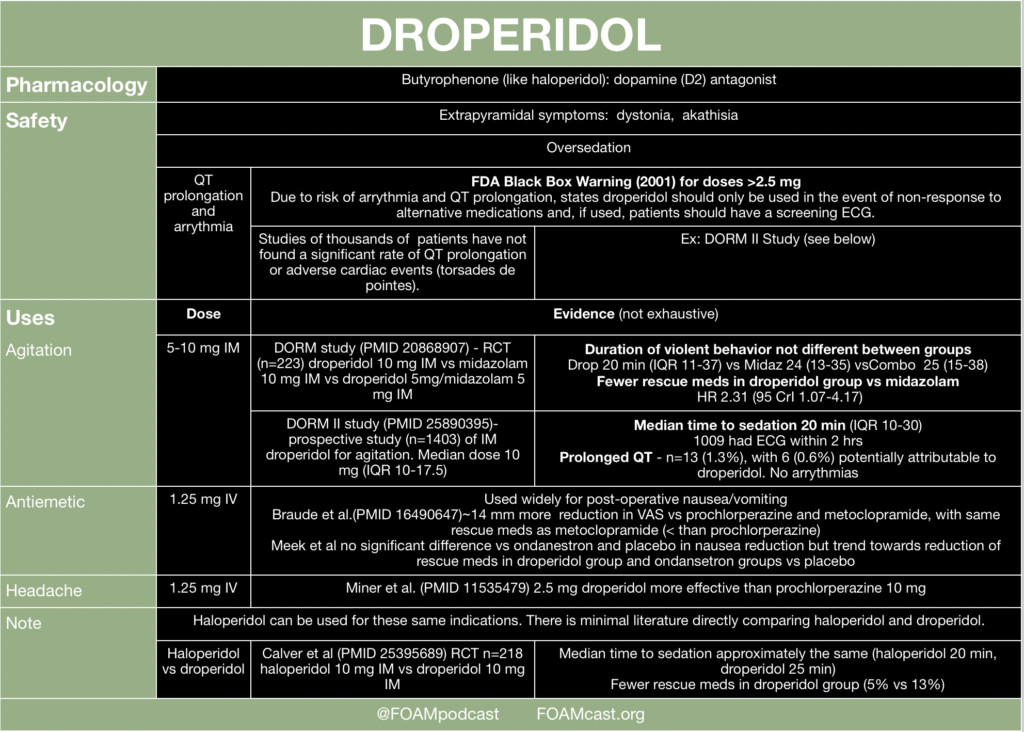
Droperidol received a black box warning from the US Food & Drug Administration (FDA) in 2001.
More on droperidol
Taming the SRU
The Short Coat
References:
Thromboelastography (TEG) or its related counterpart rotational thromboelastometry (ROTEM) have gained in popularity over the past several years. These tests assess viscoelastic clot strength in whole blood. These tests may offer more granular and potentially reliable information on the patient’s clot formation and fibrinolytic state than traditional measures of coagulation such as International Normalized Ratio (INR), partial thromobplastin time (PTT), and prothrombin time (PT).
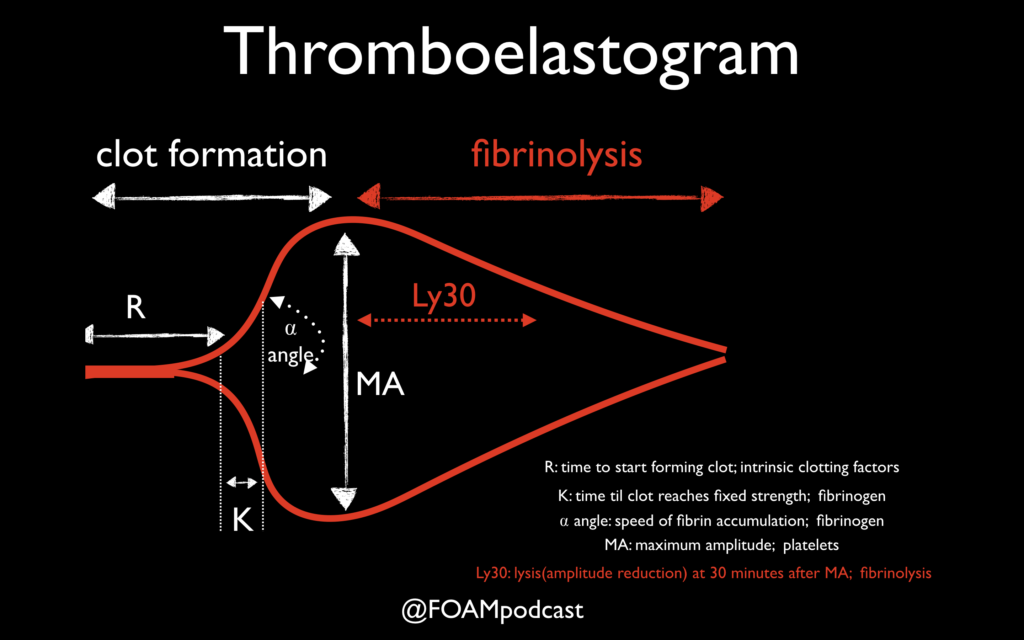
One of the primary advantages to TEG/ROTEM is the ability to target transfusion related therapies to the patient’s overall coagulation profile. Below are some common patterns that emerge and the recommended therapies.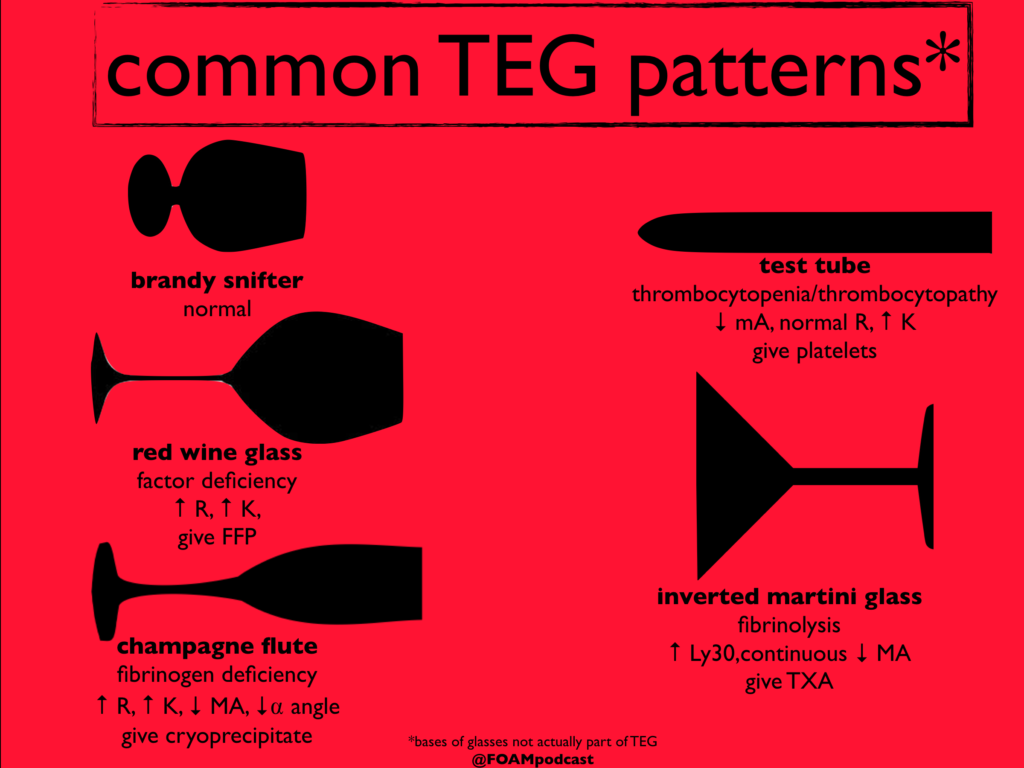
Evidence for TEG in Cirrhosis
Additional FOAM resources: PulmCrit
References:
You are called to the bedside for a postoperative patient who is hypotensive, febrile, and has acute onset of respiratory distress following the initiation of a blood transfusion. Which of the following is the most appropriate initial action in the management of this patient?
A. Apply oxygen
B. Call the blood bank
C. Order steroids
D. Stop the transfusion
[accordion]
[toggle title=”Answer” state=”closed”]
Transfusion-related acute lung injury is a blood transfusion complication characterized by a rapid onset of non-cardiogenic pulmonary edema. The pathogenesis is thought to be a two-part mechanism involving neutrophil sequestration with priming in the lung microvasculature followed by neutrophil activation by a factor in the blood product. Pre-transfusion risk factors include current smoking, chronic alcohol use, liver transplantation surgery, positive fluid balance, shock, and higher ventilated peak airway pressures. Though there is an association of transfusion-related acute lung injury with all blood products, high-plasma-volume products (plasma, apheresis platelet concentrations, and whole blood) have the greatest risk. Clinical presentation may occur immediately after the initiation of the blood transfusion although it can be delayed up to six hours. The patient may rapidly develop acute respiratory distress syndrome, with symptoms that may include hypoxemia, fever, hypotension, cyanosis, pulmonary infiltrates on chest imaging, and if intubated, pink frothy secretions when suctioned. Treatment involves immediate discontinuation of the transfusion followed by supportive care of the acute respiratory distress syndrome. This includes oxygen supplementation and hemodynamic support. Apply oxygen (A), call the blood bank (B), and order steroids (C) are treatments for transfusion-related acute lung injury but are not the most appropriate in the initial management. Discontinuing the transfusion, which is the cause of the acute lung injury, is the immediate need upon identifying the condition.
[/toggle]
[/accordion]
Risk Stratification and D-dimer in Pregnant Patients With Suspected Pulmonary Embolism (PE)
Van der pol LM, Tromeur C, Bistervels IM, et al. Pregnancy-Adapted YEARS Algorithm for Diagnosis of Suspected Pulmonary Embolism. N Engl J Med. 2019;380(12):1139-1149.
Infectious Disease Society of America (IDSA) Guidelines for Asymptomatic
Nicolle LE, Gupta K, Bradley SF, et al. Clinical Practice Guideline for the Management of Asymptomatic Bacteriuria: 2019 Update by the Infectious Diseases Society of America. Clin Infect Dis. 2019.
Benzodiazepine dosing for seizures
Sathe AG, Tillman C, Coles LD, et al. Underdosing of benzodiazepines in patients with status epilepticus enrolled in Established Status Epilepticus Treatment Trial. Acad Emerg Med. 2019 Jun 4.
Joseph B et al. Nationwide analysis of resuscitative endovascular balloon occlusion of the aorta in civilian trauma. JAMA Surg 2019. Mar 20.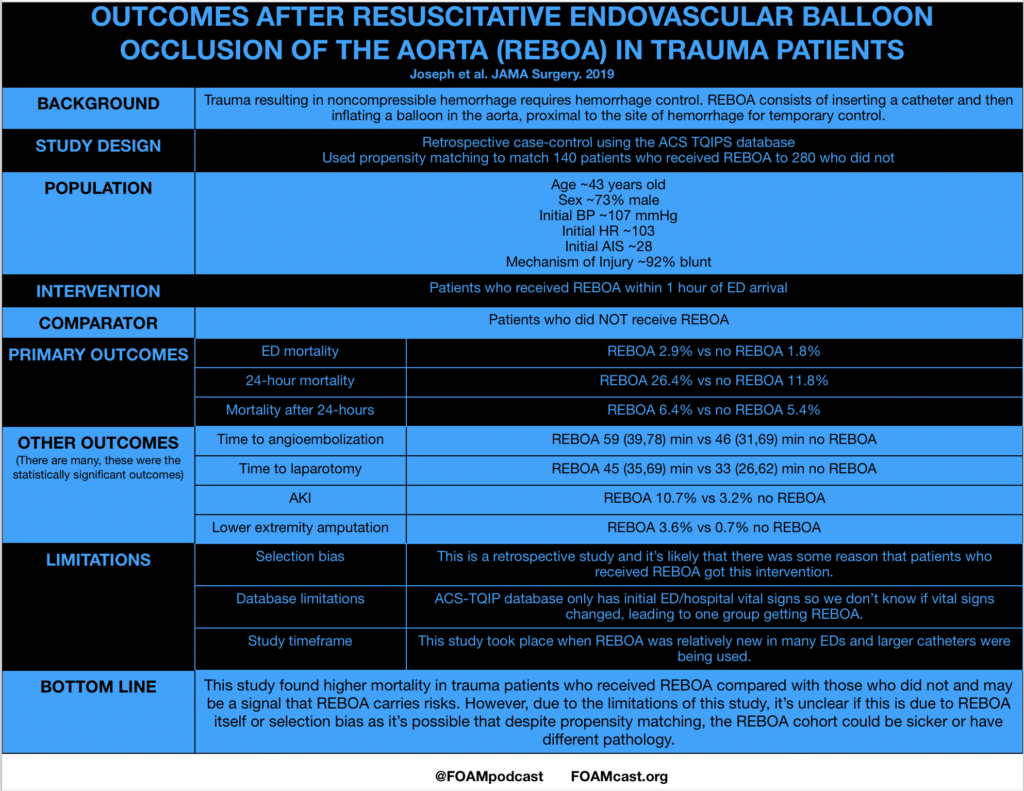
Additional References:
Psychogenic non-epileptic attacks (PNEA) have been formally referred to as pseudoseizures or psychogenic non-epileptic seizures. Recently, this entity has been rebranded to PNEA to reflect that there is no actual seizure activity and potentially prevent confusion and mislabeling among patients.
A 10-year-old girl presents with episodes of brief staring spells that she is unaware of. The patient’s mother states that the onset and termination of the spells are abrupt. The patient is otherwise healthy. She has lots of friends at school and has excellent academic performance. Physical examination and laboratory studies are normal at this time. Which of the following is the most likely diagnosis?
[accordion]
[toggle title=”Answer” state=”closed”]
[/toggle]
[/accordion]
References:
Sickle cell disease (SCD) is a terminal disease resulting from sickled blood cells caused by an abnormally folded beta-globin chain. The sickled cells cause occlusion and hyperviscosity leading to a myriad of complications. Unfortunately, some stigma associated with SCD persists in the healthcare field leading to undertreatment of pain or marginalization of patients. The American Society of Hematology (ASH) currently has draft recommendations that are open for public comment until May 13, 2019.
Which of the following is the most common cause of an aplastic crisis in a child with sickle cell disease?
A. Epstein-Barr virus
B. Parvovirus B19
C. Salmonella
D. Streptococcus pneumoniae
[accordion]
[toggle title=”Answer” state=”closed”] B. Predominantly affecting individuals of African ancestry, sickle cell anemia is a genetic disease that results in the formation of sickled red blood cells. Affected patients are homozygous for sickle hemoglobin (HbSS) which results in deoxygenated red blood cells developing a sickle or crescent shape. This leads to inflexible red blood cells, increased blood viscosity, and decreased blood flow within organs or extremities. A complication of sickle cell anemia is a transient aplastic crisis. This is caused by a short-lived stoppage of erythropoiesis, resulting in acute reductions in red cell precursors in the bone marrow, severely reduced reticulocytes in the peripheral blood, and an abrupt drop in hemoglobin level. Return to normal erythropoiesis usually occurs within two to 14 days. This transient aplastic crisis is typically caused by infection, with Parvovirus B19 being the most common etiologic agent in children. Individuals with a transient aplastic crisis are managed with transfusion. [/toggle]
[/accordion]
References:
We are at #SMACC in Sydney, Australia, thanks to the Rosh Review, delivering updates from the conference to your earbuds.
Mechanical CPR vs Manual CPR – Ken Milne vs Salim Rezaie
Massive GI Bleed and Balloon Tamponade – Dr. Sara Gray
Blakemore, Linton, and Minnesota Tube Review Video
Advocacy in Emergency Medicine – Esther Choo and Hugh Montgomery
Dr. Choo spoke about how she became an advocate and helped start TIMES UP HEALTHCARE. Check out her NEJM perspective article.
Hugh Montgomery spoke on ways to motivate individuals to change behavior by appealing to emotional aspects.